The paroxysmal event during sleep can be a diagnostic challenge as to whether it represents epileptic seizures or non-epileptic sleep disorders [1]. There are various sleep disorders with motor activity during sleep, which may mimic epilepsy. The International Classification of Sleep Disorders, 3rd edition (ICSD-3), have broadly classified nocturnal events into parasomnia, sleep related movement disorders, and sleep related breathing disorders [2]. Epileptic seizure may occur primarily in sleep or upon arousals. Among epilepsy, the nocturnal frontal lobe epilepsy (NFLE) commonly presents exclusively during sleep. Unfortunately, nocturnal paroxysmal motor activity with unusual presentation is not uncommon in clinical practice, and there have been misdiagnosis which have delayed proper treatment [3,4]. To avoid diagnostic confusion detailed history is mandatory, often times there are no recollection of the event, or information from witnesses are only limited. Further evaluation with polysomnogram (PSG) and electroencephalogram (EEG) may help diagnostic confirmation. However, despite thorough evaluation diagnostic confusion may persist. We present two cases of nocturnal repetitive motor activity with vocalization. One case of diagnostic confusion with parasomania and epilepsy, and another case with catathrenia and epilepsy.
Case Report
Case 1
A 70-year-old Korean male patient who worked as a farmer presented to sleep clinic complaining of difficulty falling asleep. He noted his sleep problems started about a year ago, and his main concern were involuntary brief shouting, which awakens him as he falls asleep.
He reported that he typically would go to bed around 11:30 p.m., and initially with no problems falling asleep. His average sleep latency was less than 5 minutes. He noted that he would wake up 3–4 times a night during first 2 hours of sleep with loud and repetitive shouting of single “Ah” syllable. Brief awakening took about 1–2 minutes to go back to sleep each time. Shouting would fade overtime, and he eventually fell asleep until morning. Occasionally, he went to the restroom, and would go through another episode of shouting before falling asleep. His final awakening would be around 6:00 a.m., and he did not feel refreshed upon awakening. He estimated that on average he was sleeping five hours per night. He denied any history of seizures. Before visiting the sleep clinic, he first consulted his psychiatric physician and was diagnosed with period limb movement disorder and treated on clonazepam 0.5 mg, but overnight PSG was not done. The clonazepam before bedtime partially relieved the symptoms, but repeated awakening by involuntary shouting during entry into sleep persisted. He had other medical problems of hypertension, diabetes mellitus, hyperlipidemia, chronic kidney disease, cerebral artery stenosis, arrhythmia on implanted pacemaker, liver cirrhosis and dementia.
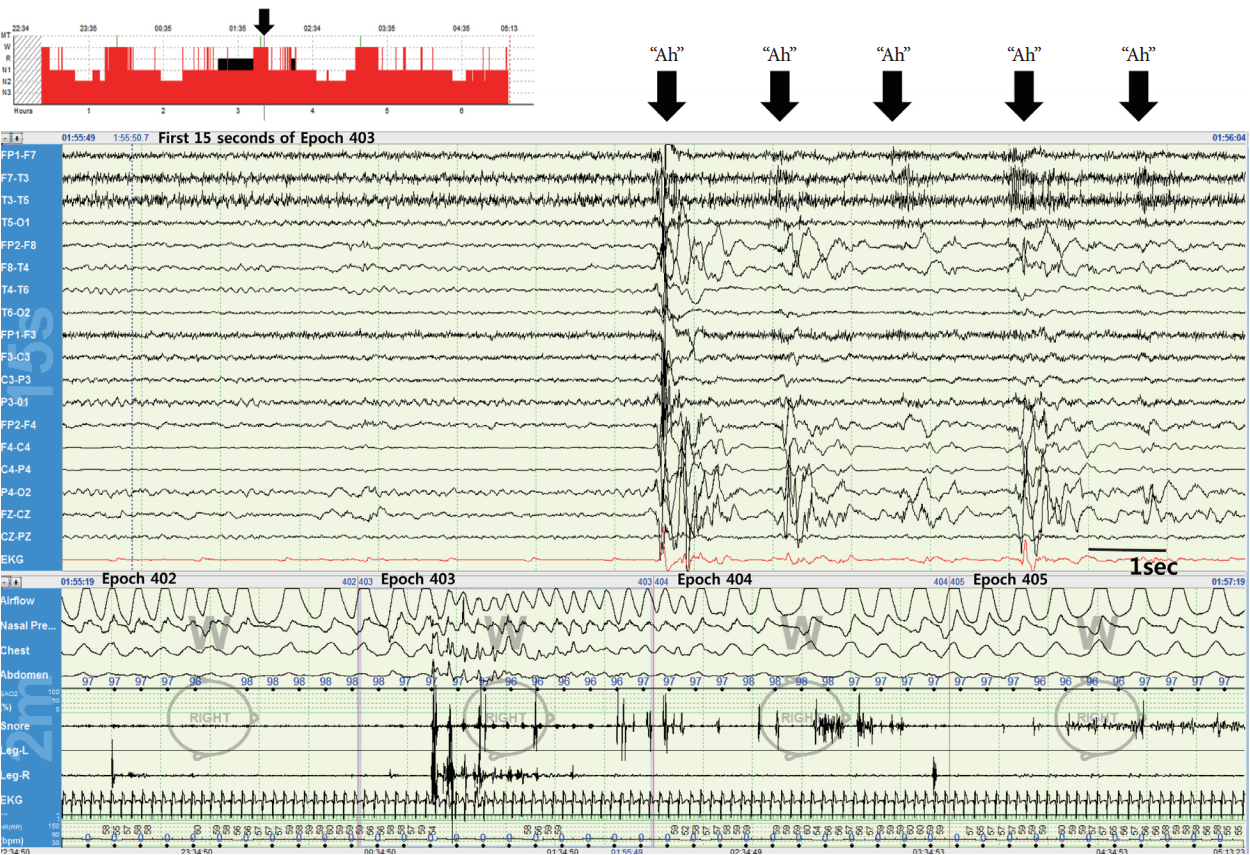
His body mass index was 25.91 kg/m2. The neurological examination, and brain MRI were unremarkable. He underwent PSG with expanded EEG and found to have total sleep time of 4 hours 57 minutes, and sleep latency of 6.5 minutes (Fig. 1). PSG also revealed moderate obstructive sleep apnea with an apnea-hypopnea index (AHI) of 22/h. The periodic limb movement index was 3.6/h. He had more than 40 “Ah” events during sleep. Most of the events was during first two hours of sleep, and it gradually faded as sleep deepens. Most events occurred as he falls asleep or soon after initiation of sleep. The events were repetitive, stereotyped motor behavior involving muscles of vocalization. He would shout repetitive single “Ah” syllable four to five times semi-rhythmically. Most events were during non-rapid eye movement (NREM) sleep, but one episode was during rapid eye movement (REM) sleep. EEG was obscured with muscle artifacts during the events, and no significant epileptic discharges were seen. Although, EEG was suboptimal to differentiate epileptic seizures with sleep disorders, we have considered possible nocturnal epileptic seizure. While taking clonazepam, he started topiramate 50 mg before bedtime. His symptoms gradually subsided, and he reported only minimal symptoms persisted, which no longer bother him during sleep. For a year, he reported that symptoms would come back when he forgets to take his clonazepam and topiramate.
Case 2
A 54-year old Korean male patient lives in Papua New Guinea presented to sleep clinic complaining of awakening during sleep with sense of hard to breath. He felt something is stuck in his airway, and prevented him to breathe normally. He noted his sleep problems started about three months ago.
He reported that he has not been a very good sleeper since his thirties, recently with these new symptoms he complained that his sleep got event worse. He usually goes to bed around 12:00 a.m., and takes about two hours to fall asleep. When he woke up at 7:00 a.m., he felt he had slept for only four hours. He noted that he would wake up 3–4 times a night, however he did not recognize the causes of awakening. He denied any history of seizures, or other sleep disorders. He had surgical treatment for chronic sinusitis 15 years ago, but no other medical problems.
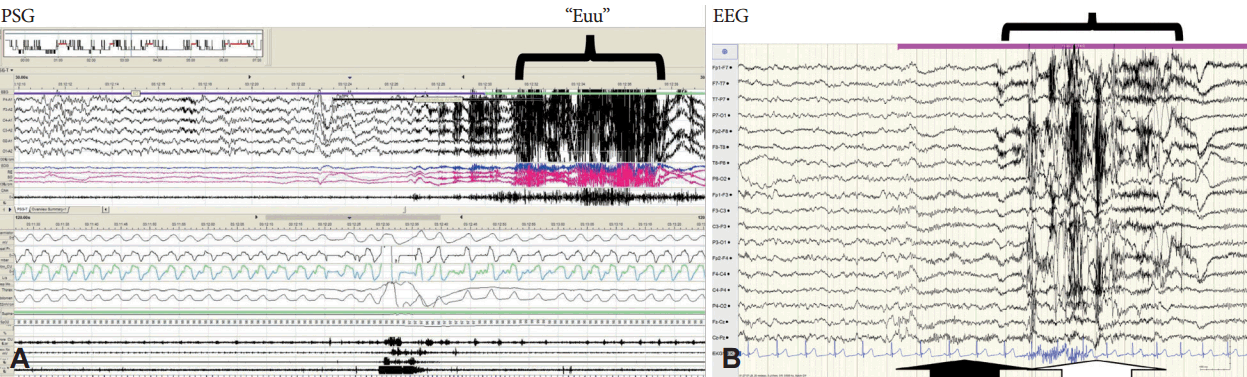
His body mass index was 24.03 kg/m2. The neurological examination, and brain MRI was unremarkable. He underwent PSG due to concerns about sleep related breathing disorders. The PSG revealed total sleep time of 6 hours 38 minutes, and sleep latency of 8 minutes (Fig. 2). PSG also revealed AHI of 4.6/h. Arousal index was markedly increased to 21.8/h. He had 13 events during sleep. With no preceding sleep events, he would wake up and for three to nine seconds he would toss and turn, elevate his arm, touch his nose, or eyes, scratch his neck and turn his head for few seconds. Following these brief motor behaviors, he would make long monotonous “Euu” sound with stretch which last for two to five seconds. He falls back to sleep following the events. These events were seen during NREM sleep and REM sleep. He did not recollect these events in the morning. The vocalization of the events was suggestive of catathrenia of sleep related breathing disorders, but unusual motor behavior preceding the vocalization questioned possible epileptic event during night. He underwent video EEG (VEEG) monitoring in the epilepsy monitoring unit (Fig. 2). During three days of monitoring, on average there were two events per hour of sleep. Each event was similar to each other. Definite EEG changes were not shown due to movement artifact. However, atypical fast activities were preceded for 3–4 seconds before awakening were found in some episodes. It may suggest the possibility of epileptic seizures though definite ictal rhythms were not demonstrated during the event. Interictal epileptiform discharges were not noted. He was given valproate 900 mg per day, and clonazepam 0.5 mg before bedtime on second day of monitoring, but frequency had not changed. Just severity of clinical presentation seemed to be lessened; duration of events became shortened. During PSG and VEEG, chocking ‘hard to breath’ event was not seen, but unusual motor activity with vocalization were seen several times during night. These events attributed to frequent arousal, and may have attributed to poor sleep. We are still in confusion with this nocturnal event, but considering frequent arousal and involuntary movement during sleep, he was started on lorazepam 0.5 mg and clonazepam 0.75 mg before bedtime. He reported his sleep is better on medications. Any changes of “Euu” vocalization was not confirmed since he cannot recall the events.
Discussion
It is not uncommon to encounter difficult case to distinguish a nocturnal epilepsy form a non-epileptic sleep disorder. Both may occur selectively during sleep with increase in motor and autonomic activity with a change in the level of consciousness [5]. This report has described two adults of unusual motor phenomenon during sleep that lead to significant sleep disturbances.
First case was unclear whether events were occurring as he entered sleep and awakened by the shouting or arousal from sleep precedes the shouting. According to ICSD-3, parasomnias are undesirable physical events or experiences that occur during entry into sleep, within sleep, or during arousal from sleep [2]. Parasomnias, depends on sleep stage it may occur, is defined as NREM, or REM parasomnias. NREM parasomnias are arousal disorders which most commonly seen in childhood, but there are less than 5 percent that persist into adulthood [6]. Clinical presentation many vary with confusional arousal, sleep walking, sleep terrors, however they share common features of confusion and disorientation during the event. In general there is poor recollection of the event, and perceiving the event as sleep disturbing can be unusual, as in our case [7]. REM sleep behavior disorder (RBD), a parasomnias occurring during REM sleep in adults have motor activity during sleep. However, RBD patients report intense, vivid and often violent dreams, as it occurs during REM sleep. Our patient had events during NREM, and REM sleep stage as documented by PSG, but most of the events were assembled during first two hours of sleep. Moreover, REM sleep without atonia, which is a diagnostic PSG finding of RBD were not seen. NREM parasomnia, as the definition states, events would appear during NREM sleep, especially during slow wave sleep of first third of the sleep period [8]. The frequency of events are occasional, typically 1–3 times per month [9]. Old age of onset, stereotyped presentation, occurring both in all sleep stages, and clustering during night suggested possible diagnosis of nocturnal epileptic seizure. As for NFLE, the mean age of onset is 14 years, but with wide range of 1–64 years [7]. NFLE seizures clusters, typically three to eight events during single night [1]. About 30% also have seizures during daytime, some will have occasional secondarily generalized tonic clonic seizures, which helps to differentiate from sleep disorders. However, remaining majority presents only during sleep and simple or complex partial seizures [7]. Seizure in NFLE have been demonstrated to occur during stage 2 NREM sleep [7,10]. Epileptic seizure may resemble parasomnias with confusion and disorientation, but dystonic posturing can suggest seizures [7]. Our patient only manifested loud short repetitive vocalization. While vocalization is common in both NFLE, and parasomnias as shouting, screaming and incoherent speech, but repetitive single syllable have not been reported in epilepsy nor in sleep disorders. With big diagnostic confusion, we have considered most significant clinical feature of the stereotyped presentation. Based on this suggestions, we diagnosed with possible epileptic event, and tried antiepileptic drug, which responded optimally. It needs close clinical follow up to elucidate our diagnosis.
Our patient presented was episodes of respiratory difficulty episodes during sleep, although PSG and VEEG did not record the episode, the respiratory index was normal. On the other hand, recurrent nocturnal groaning sound during sleep was seen, which patient has no recollection of the events. These events were associated with high arousal index. Catathrenia is a rare sleep disorder, also known as nocturnal groaning occurring during sleep with average age of 33 years at diagnosis [2]. While snoring usually occurs during inspiration, catathrenia makes monotonous vocalization resembling groaning during prolonged expiration following deep inspiration. The differential diagnosis of this unusual sound during night includes epileptic seizure. There are cases of epilepsy, which later on PSG study revealed no epileptic discharges, but catathrenia [1]. The PSG findings showed each episode was associated with bradypnea without evidence of respiratory effort, resembling central sleep apnea during groaning sounds. These vocalization occur in clusters, more commonly during REM sleep stage, 63.3% of the events were associated with arousals, and in 94% of them an arousal occurred before or together with the onset of bradypnea [2]. Our patients had groaning sound during sleep, but not so much like catathrenia. The groaning sound occurred mostly few seconds after the arousal, and this accompanies other motor behaviors including large stretch. Further on respiratory monitoring did not show loss of respiratory effort. The VEEG did not show definite epileptic seizure, but preceding fast activity of both parasagittal channels did suggest the epileptic seizures combined with sleep disorders. The patient reported sleep got better on lorazepam 0.5 mg and clonazepam 0.75 mg, however we are not sure whether these events actually subsided as sleep got better on hypnotics, or seizure subsided with benzodiazepine anti-seizure effects.
Nocturnal motor activity can be very confusing for some cases. Detailed history, PSG and EEG might help, but similarity of the non-epileptic events to epileptic seizures may be very challenging even for sleep specialist, and epileptologiest.